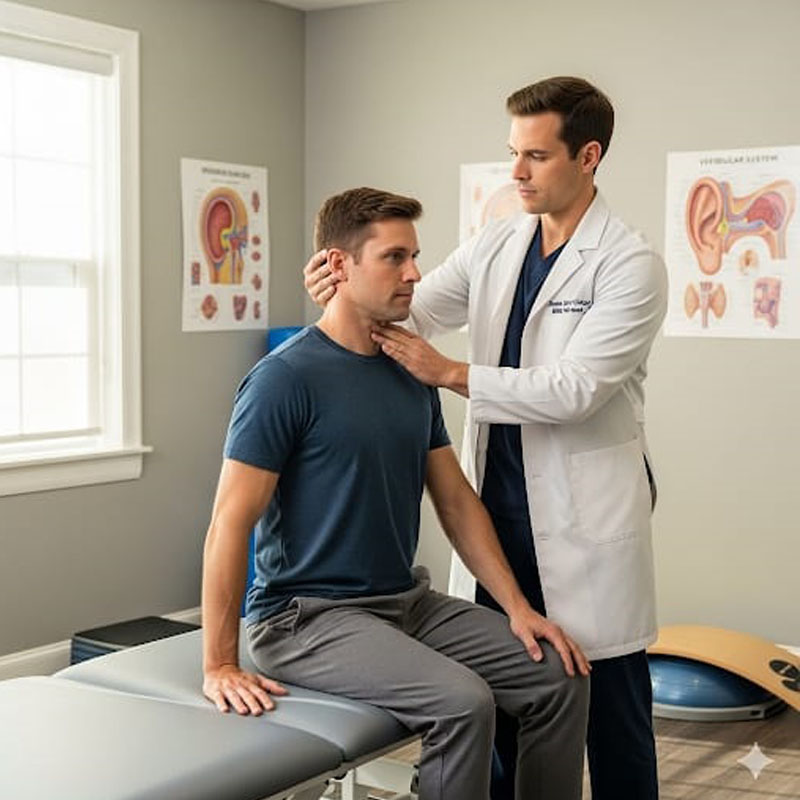
Athlete training at MHC encompasses much more than just traditional strength and conditioning. The advanced scientific concepts of movement analysis, energy system development, and performance testing form the foundation of our sport-specific programs. Our programs, which are tailored to each athlete’s sport and goals, provide: Detailed biomechanical and movement assessmentsRegular exercises for strength, power, and conditioningTraining for plyometrics, agility, and speedStrategies for injury prevention and functional movement correctionRecuperation, renewal, and performance evaluationTo maximize training loads, lower the risk of injury, and guarantee peak performance at the appropriate times, we employ data analytics and real-time feedback. Every athlete at MHC receives professional, tailored, and morally sound care, whether they are recovering from an injury or trying to set new records. This supports our conviction that every accomplishment is a turning point in human care.
Stroke Rehabilitation
Person-centered goals, interdisciplinary teamwork, and evidence-based treatment are the cornerstones of MHC’s stroke rehabilitation program. Intensive and task-specific motor retraining (upper and lower limb) is part of our strategy.Retraining gait and balance, including the use of contemporary technologies (such as virtual reality, robotics, and treadmills)Mirror and constraint-induced therapyBehavior, speech, and cognitive therapyEducation and fatigue management for reintegration into community activitiesIn order to establish and accomplish significant milestones in functional independence, social participation, and enhanced quality of life, MHC clinicians work in tandem with patients and their families. As long as rehabilitation yields significant results, it will continue, demonstrating our steadfast dedication to milestone-focused, lifelong human care.
Parkinson’s Rehabilitation
MHC’s evidence-based, multidisciplinary Parkinson’s Disease (PD) rehabilitation program maximizes movement, safety, and involvement for people with PD at every stage. Our programs consist of: Using cueing, rhythmic exercises, and gradual task practice, we retrain mobility, gait, and balance. Functional movement techniques to control transfers, postural instability, and frozen Exercises for voice, strength, flexibility, and aerobics Instruction and assistance for caregivers, self-management, and lifestyle modification Each level of therapy is unique. whereas mid-stage therapy targets specific impairments, advanced-stage care concentrates on comfort and key functions, whereas early intervention delays disability and preserves activity. In keeping with our milestone-driven philosophy, empowerment and functional independence are always the end goals.
Vestibular Dysfunction Rehabilitation
MHC’s Vestibular Dysfunction Rehabilitation offers patients with balance system problems, such as unilateral or bilateral vestibular hypofunction, labyrinthitis, and vestibular neuritis, complete care. Gaze stability exercises are incorporated into our programs to enhance visual concentration when moving the head. Exercises for habituation to reduce dizziness caused by symmetry Training for balance and gait to improve stability Significant reductions in dizziness, decreased risk of falls, and improved functional abilities are among the results. The vestibular treatments offered by MHC are highly customized, evidence-based, and assist clients in regaining their active, milestone-filled lives.
Vertigo Rehabilitation
The Vertigo Rehabilitation therapies offered by MHC address balance issues and dizziness brought on by neurological disorders, traumatic injuries, or central or peripheral vestibular dysfunction. Based on a comprehensive evaluation, treatment is customized and may involve exercises for balance retraining, habituation, and gaze stabilization. The following are the goals of vestibular rehabilitation: Encourage compensation in the balancing system (neuroplasticity) Minimize vertigo and regain mobility confidence Reduce the chance of falls and avoid losing your independence. Physiotherapists with advanced vestibular treatment training implement protocols at MHC, which are supported by research. In keeping with our patient-centered purpose, patients receive personalized home programs, progress monitoring, and coping mechanisms for everyday obstacles, guaranteeing a comprehensive recovery.
BPPV Rehabilitation
A frequent vestibular condition that causes severe, abrupt-onset vertigo is called Benign Paroxysmal Positional Vertigo (BPPV). Through techniques like the Epley Canalith Repositioning Procedure, which is acknowledged globally as the gold standard for treating this problem, MHC provides skilled BPPV rehabilitation. Tiny crystals inside the inner ear are displaced in BPPV, which causes aberrant stimulation and incapacitating vertigo when head position changes. Our experienced therapists can safely perform canalith repositioning operations to restore normal inner ear function and accurately identify BPPV utilizing positional testing. Inform patients about self-management techniques and post-procedure safety measures. Most patients who receive BPPV treatment at MHC see quick, noticeable improvement, which reduces their risk of falling and downtime. Our dedication to a prompt, milestone-driven resolution of life-altering illnesses is reaffirmed by thorough follow-up, which addresses any recurrence and promotes long-lasting recovery.
Fitness Training
MHC’s fitness training integrates exercise prescription for general health, preventive, and rehabilitation, and is based on the scientific principles of physiotherapy. Our fitness programs emphasize progressive resistance and aerobic training, personalized evaluation, and goal-setting, which go beyond traditional gym exercises. Improved posture, balance, and flexibility Exercises that are functional, sport-specific, and injury-prevention Instruction on community-based and at-home activities. Improved cardiovascular health, flexibility, injury resistance, mental wellness, and functional independence are just a few of the many advantages. Whether a patient is pursuing sports success, managing a chronic illness, or recuperating from an injury, MHC’s fitness training services open the door to an active, healthy, and sustainable lifestyle. Our goal of establishing benchmarks for the best possible human care and performance is directly fulfilled by this service.
Women’s Health Programs
For problems specific to women at every stage of life, including as pregnancy, postpartum, menopause, pelvic discomfort, and post-surgical treatment, MHC’s Women’s Health Programs provide specialist physiotherapy. These services, which are provided by medical professionals skilled in female anatomy and physiology, cover: Dysfunction of the pelvic floor (pain, prolapse, incontinence) Musculoskeletal discomfort during pregnancy and after giving birth (back, pelvis, sciatica) Management of menopause (muscle stiffness, joint discomfort) Recuperation following breast or gynecological surgery. Customized exercise plans, manual therapy, pelvic floor rehabilitation, breathing and relaxation methods, and lifestyle education are all part of the treatment. In order to provide individualized and goal-focused treatment, a strong emphasis is put on privacy, compassion, and collaboration with each woman. These programs help women reclaim their self-esteem, independence, and control over their health, whether it is improving their quality of life after menopause, managing chronic pelvic pain, or starting to exercise again after giving birth. MHC’s dedication to women’s health is a reflection of our goal to offer each person inclusive, milestone-oriented care.
Behavioral Therapy
The biopsychosocial model and behavioral medicine concepts form the basis of MHC’s behavioral treatment program in physiotherapy and rehabilitation. This method acknowledges that changing health-related behaviors, attitudes, and coping mechanisms is frequently necessary for long-lasting physical health improvement, particularly for patients who have chronic pain, ongoing musculoskeletal problems, or psychological obstacles to recovery. Interventions for behavior modification might involve: Setting goals together, keeping track of patients’ progress using digital tools and a journal, providing feedback, encouragement, and motivational interviewing. Plans for graded activities Cognitive-behavioral strategies to address self-efficacy, anxiety avoidance, and pain catastrophizing These techniques are used by MHC therapists to encourage the best possible involvement, adaptability, and resilience—all of which improve mental and physical health. MHC maintains its dedication to patient empowerment, handicap reduction, adherence to health-promoting habits, and reaching milestones in daily involvement by incorporating behavioral therapy into all facets of treatment.
Speech Therapy
The goal of MHC’s speech therapy program is to assist people who struggle with language, communication, voice, swallowing, or speech clarity as a result of stroke, neurological illnesses, trauma, or developmental issues. Our speech-language pathologists are prepared to use evidence-based assessment and intervention techniques with both adults and children. The following problems are frequently treated: voice abnormalities, apraxia of speech (problem with motor planning), dysarthria (motor speech disorder), aphasia (language impairment), and dysphagia (difficulty swallowing). Restoring or improving speech output, clarity, and understanding are the goals of therapy. Instruct students in alternate forms of communication, such as written correspondence, augmentative devices, and gestures. Teach caregivers and families helpful techniques. Boost the effectiveness and safety of swallowing A comprehensive, respectable, and customized approach is used in professional speech therapy. The therapists at MHC customize programs based on the skills and objectives of each client, using practical communication activities, repetition, and stimulation to promote successful improvement. In keeping with our principles, we prioritize functional rehabilitation, encourage patient autonomy, and communicate with compassion, enabling clients to regain their lives and their voices.